Managing Breast Engorgement:
A Practical Guide
Essential Strategies to Minimize Swelling and Maintain Milk Flow
This guide helps you understand and manage breast engorgement. It offers step-by-step instructions and strategies to help ease engorgement discomfort and promote successful breastfeeding.
What’s in this guide?
Who is this guide for?
This guide is for anyone who is breastfeeding and experiencing breast engorgement.
Who are we?
We are The Lactation Collection (TLC), a team of Internationally Board Certified Lactation Consultants (IBCLCs).
How do we use this guide?
We use this guide for after-consult care instructions. This guide serves as a supplementary tool to reinforce the support and recommendations provided during your consult.
Understanding breast engorgement
Breast engorgement is a common experience, but it is helpful to understand why it happens. It occurs when the breast tissue becomes overfilled. This isn’t just because of milk; it is also caused by an increase in blood and other fluids rushing to the area.
Engorgement typically happens between two and five days after your baby is born.
While some fullness is normal as your milk volume increases, it can become a problem if it makes it hard for your baby to latch or causes you significant pain.
Signs & symptoms
If you are experiencing engorgement, you might have:
- Firm, swollen breasts
- Pain or discomfort during feeding
- Breast tissue hardness of (feeling like the tip of your nose or forehead)
- Extended Swelling: In some cases, engorgement may extend into the armpit area, indicating that the fullness and swelling can involve more than just the breast tissue
- Nipple Alterations: Engorgement may cause the nipples to flatten or change shape, which can affect your baby’s ability to latch properly

Preventing Engorgement: Do’s and Don’ts
Managing engorgement starts with a few proactive steps. By following these “dos and don’ts,” you can often keep swelling under control and ensure your baby gets enough milk.
Things to do to help prevent breast engorgement
- Begin feeding as soon as possible after delivery
- Aim to breastfeed 8–12 times during the first 24 hours to ensure the breasts are emptied and to prevent overfilling

- Use techniques from the “Positioning and Latch Checklist” to achieve a deep, effective latch
- Bring the baby to your breast (not the breast to the baby) to help facilitate a natural, proper latch
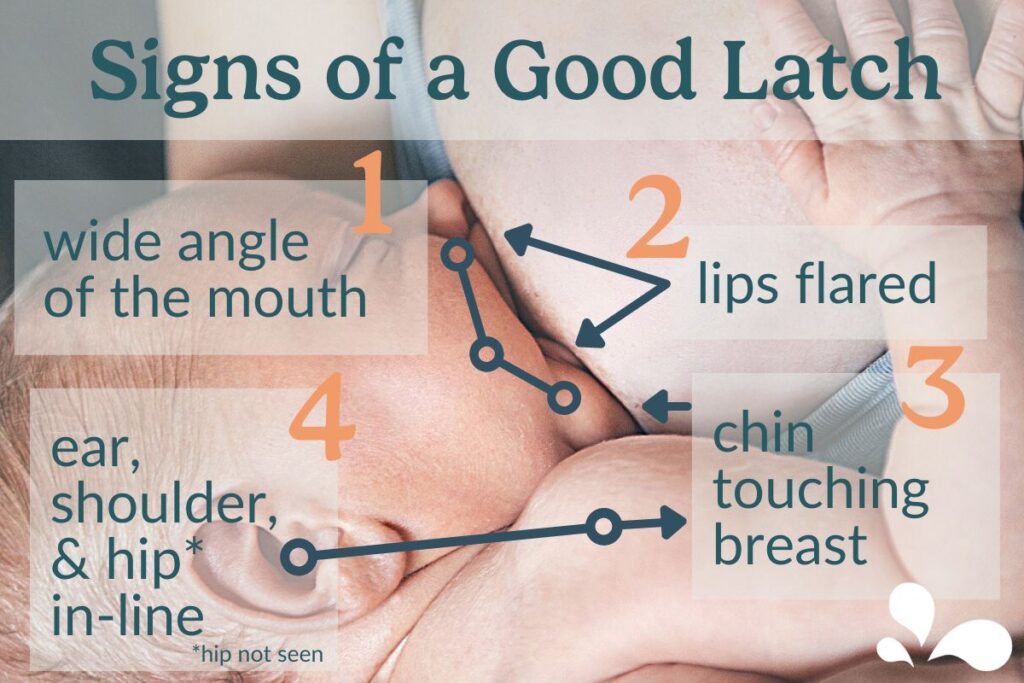
- Do not skip feedings; respond consistently to your baby’s hunger cues
- If necessary, supplement with hand expression to fully empty the breasts

- Limit or avoid supplementing with formula early on to maintain the natural supply/demand balance, which is key in regulating milk production and preventing engorgement

Things not to do to help prevent breast engorgement
EARLY
- Opening mouth
- Light sucking motions
- Tongue extension
- Rooting behavior
- Turning head side to side
- Sucking on anything nearby
MID
- Bringing hands to face
- Light sounds or whimpering
- Body wriggling
- Body flexion
LATE
- Fussy
- Agitated body movements
- Crying
- Turning red
Engorgement management techniques
If you are already experiencing discomfort, there are several techniques you can use before, during, and after feeding to find relief.
Pre-Feeding Techniques
Cold compresses are recommended for reducing swelling, pain, and inflammation.

Warm compresses may feel soothing, but can worsen engorgement for some due to increased blood flow; a warm compress can help with minor engorgement, but avoid using warmth for extreme engorgement.

Use your fingertips to gently massage the breast from under the nipple toward the armpit, then stroke from the outer breast toward the nipple. This can help break up areas of stiffness.
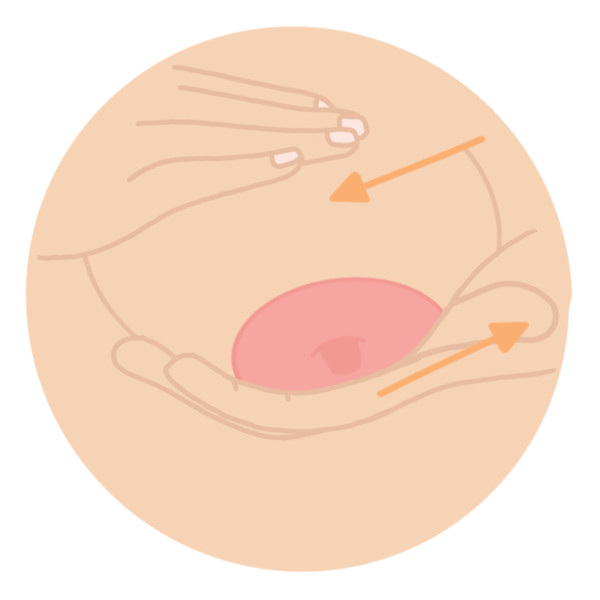


- Use chilled cabbage leaves to help reduce swelling before feedings
- Apply for 15-30 minutes, but be cautious not to overuse as it may decrease milk supply
- Can be used 2-3 times daily; stop use immediately once engorgement has lessened
- Do not use if allergic; be sure to test a small area if you have skin sensitivities


Techniques During Feeding
Achieving an Effective Latch
- Ensure the baby latches deeply; check that the latch is asymmetrical: more of the areola visible above the baby’s top lip
- Make sure that your nipple is free from pinching or creasing
- See the “Positioning and Latch Checklist” for step-by-step instructions

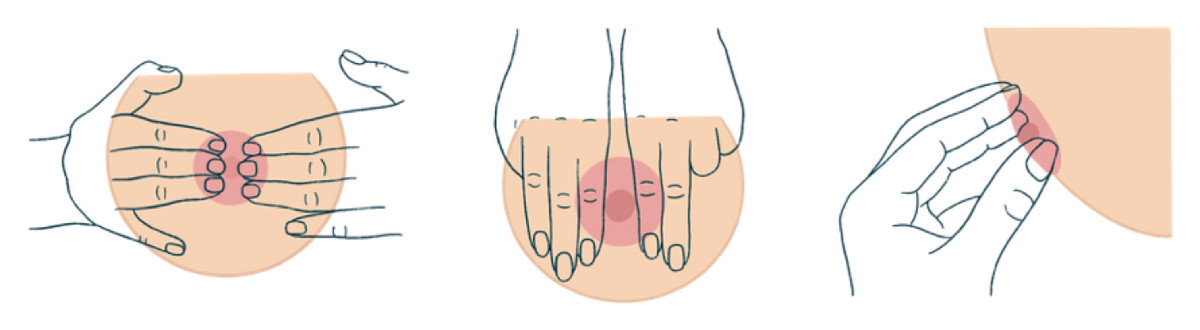
Reverse Pressure Softening (RPS)
- Practice the RPS technique to help ease nipple protrusion.
- If discomfort occurs, a small dose of an over-the-counter pain reliever can help (consult a provider before use)
- Watch this Reverse Pressure Softening video for visual guidance
Hand Expression as Needed
- If the baby is having trouble latching due to full breasts, use hand expression briefly before feeding but after reverse pressure softening to make the nipple more accessible.
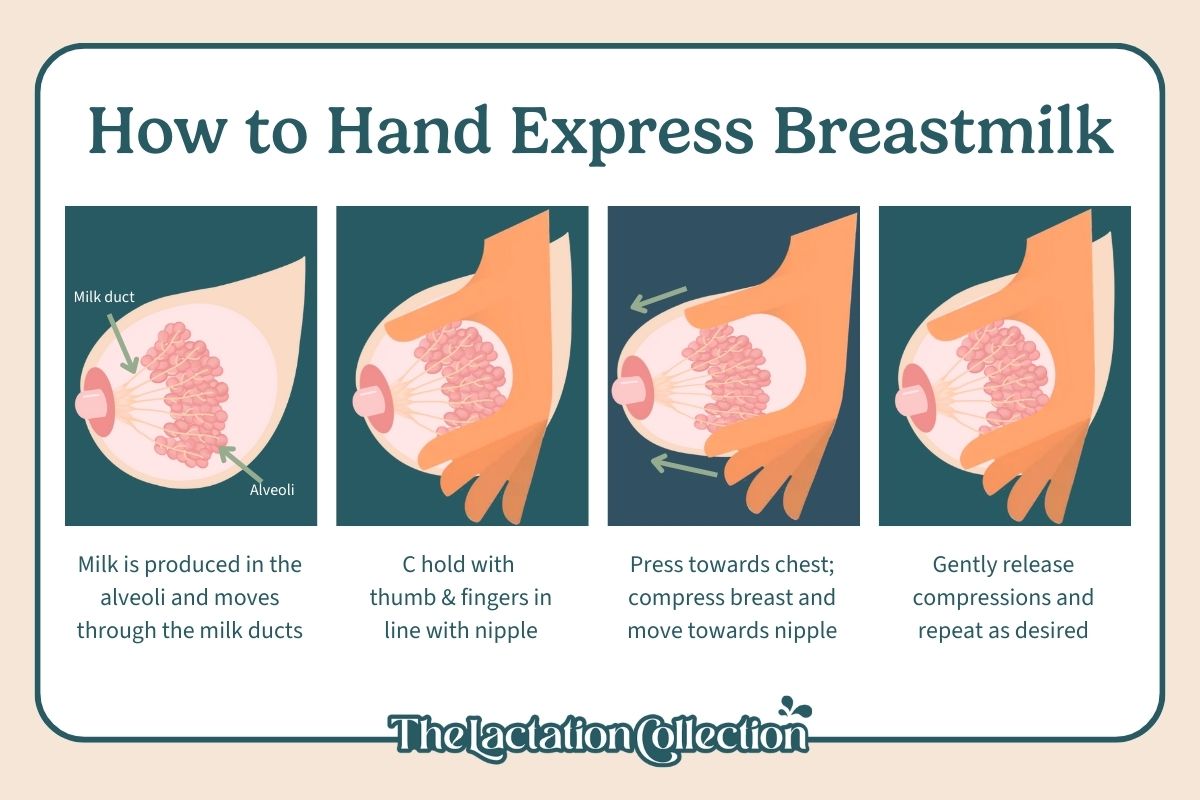
Post-Feeding Care
Cold Compress Application
- After feeding, apply a cold compress (an ice pack or a bag of frozen vegetables wrapped in a towel) for 10–20 minutes to reduce swelling
- The compress should be wrapped in a cloth to protect the skin
- Follow proper technique for applying cold

Additional Self-Care
- Rest on your back to help reabsorb excess fluid
- Consider a gentle massage after feeding
- Monitor for any ongoing pain or discomfort
- Maintain self-care routines to prevent recurrence


Quick Checklist Summary (Appendix)
Pre-feeding care
The goal before feeding is to reduce swelling so the milk can flow and the baby can latch.
- Cold compresses: Apply cold packs to reduce inflammation and pain
- Lymphatic massage: Use gentle, light touches to massage the breast skin toward the armpit to help drain excess fluid
- Cabbage leaves: You can apply chilled cabbage leaves to the breast for 15–30 minutes to reduce swelling, but use them cautiously as overuse can lower your milk supply
- Medication check: If pain is significant, ask your healthcare provider about using an over-the-counter anti-inflammatory (like ibuprofen) to help reduce swelling and discomfort
During feeding
- Check the latch: Ensure the baby has a deep, asymmetrical latch where more of the areola (dark skin) is visible above their top lip
- Reverse pressure softening (RPS): If the areola is too hard for the baby to grab, gently press inward around the nipple to push fluid back and soften the area
- Hand expression: If the breast is still too full, hand express a small amount of milk to soften the tissue before bringing the baby to the breast
Post-feeding care
- Cool it down: Apply a cold compress or ice pack (wrapped in cloth) for 10 to 20 minutes
- Rest position: Lie on your back when resting to help gravity drain excess fluid back into your body
- Gentle touch: You can perform a very gentle massage to help relax the tissue
After the baby is done, focus on comfort and reducing inflammation.
When to seek medical attention for engorgement
While some fullness is expected, severe engorgement can lead to other issues.
It is important to know when to stop self-treating and reach out to a professional.
Early intervention is the best way to resolve these issues and continue your breastfeeding journey successfully.
Warning signs
- Pain that does not go away after trying the techniques above
- Your baby is unable to latch or is not feeding well
- Symptoms of mastitis or infection: a fever, red streaks on the skin, chills, or body aches
Action steps
If you notice any of these warning signs, do not wait.
Follow this timeline for support:
- Less than 24 hours of symptoms: Contact your IBCLC for management help
- More than 24 hours of symptoms: Contact your OB, Midwife, or Primary Care Provider to rule out infection.
Remember, persistent pain is not normal.
Early intervention is key. If you experience signs of infection (such as fever, chills, or red streaks) or if your baby is unable to latch despite using these techniques, do not hesitate to reach out to your IBCLC or healthcare provider immediately.
Additional resources
We hope this guide helps you feel more confident in managing breast engorgement. Below are links to additional resources that will you help you.
- Reading resources
- Reverse Pressure Softening Video


